In Memoriam: Martin C. Mihm Jr., MD, Department of Dermatology
 Brigham and Women’s Hospital mourns the loss of Martin C. Mihm Jr., MD, a physician, researcher and educator in the Department of Dermatology whose groundbreaking discoveries have saved lives and whose lifelong commitment to mentorship influenced generations of clinicians in the fields of dermatology, dermatopathology and pathology. He died on July 19, 2022 of a sudden illness at age 88.
Brigham and Women’s Hospital mourns the loss of Martin C. Mihm Jr., MD, a physician, researcher and educator in the Department of Dermatology whose groundbreaking discoveries have saved lives and whose lifelong commitment to mentorship influenced generations of clinicians in the fields of dermatology, dermatopathology and pathology. He died on July 19, 2022 of a sudden illness at age 88.
An international expert on malignant melanoma, Dr. Mihm helped shape the way skin cancers are identified and diagnosed, and his discoveries and insights influenced the way these tumors are ultimately treated. Notably, he established the importance of tumor-infiltrating lymphocytes — a type of cell that can recognize and destroy cancer cells — in contributing to the prognosis of patients with primary and metastatic melanoma. He also collaborated with the late melanoma expert Wallace Clark, MD, to create the current clinical categories for melanoma: superficial spreading, nodular, acral lentiginous and lentigo maligna.
“This is a man who has saved countless lives, and I am forever grateful for the degree to which he has enhanced my own life as a mentor and friend,” said Dermatology research colleague Tobias Schatton, PharmD, PhD, who recently partnered with Dr. Mihm on a melanoma study. “Martin set the prime example of how to live with integrity and purpose.”
In addition to his tremendous contributions to science and medicine, Dr. Mihm had an equally profound impact on others with his joyful spirit.
“Beyond his credentials, accomplishments, publications and degrees, Marty was a warm, funny, kind and generous man,” said Thomas Kupper, MD, chair of Dermatology. “His enthusiasm was palpable and infectious. He could make a microscope slide image come alive with subtle insights that, once pointed out, were obvious. He was also considerate, taking time to know the names of all the residents and students in the program and to learn about people around him. He truly was one of a kind — the sort of character who comes along rarely, like a comet leaving light and brilliance in his wake.”
Colleague and friend Jennifer Lin, MD, director of the Melanoma Risk and Prevention Clinic, reflected that Dr. Mihm was always ready to share his experiences and words of encouragement with those around him.
“He had a kind word for everybody,” Lin said. “His enthusiasm and positivity were contagious — and made coming to work so wonderful.”
Dr. Mihm’s passions for life and medicine often intertwined. Lin recalled that Dr. Mihm and Dr. Clark named the “superficial spreading” category of melanoma after sharing the morphological pattern of this lesion with students from the Boston’s Museum of Fine Arts and learning of a painting with similar morphology.
“That he could share his gifts and brilliance with us was a truly wonderful experience, and we are all better for it,” said Kupper.
Dr. Mihm was dedicated to promoting education and mentorship throughout his career. Beginning in 1974, he served as chief of the Massachusetts General Hospital Dermatopathology Unit, where he founded one of the first five dermatopathology training programs in the United States. In 1993, he joined the faculty of Albany Medical Center to establish a new dermatology and dermatopathology training program there.
“Through his mentorship and training for generations of residents, fellows and faculty, Martin’s impact will continue to grow exponentially,” Schatton said.
Beginning in 2010, Dr. Mihm served as director of the Melanoma Program in Dermatology and the Dana-Farber Brigham Cancer Center. He was also the founding director of the Mihm Consultative Service in Dermatopathology.
Over the course of his career, Dr. Mihm’s commitment to patient care inspired his work to make health care, particularly cancer treatment and prevention, more widely accessible. He was a co-founder of the Rare Tumor Institute of the World Health Organization in Milan, Italy, before acting as its external coordinator for five years, and he also helped establish clinics in Albania, India, Italy, Russia and Vietnam. Most recently, he served as co-director of the European Organisation for Research and Treatment of Cancer’s Melanoma Pathology Program.
Adriano Piris, MD, co-director of the Mihm Cutaneous Pathology Consultative Service, met Dr. Mihm after coming to Massachusetts General Hospital for his first dermatopathology rotation. Dr. Mihm soon became an important force in his life, as an inspiring mentor and a dear friend. Piris was honored to eventually work with Dr. Mihm as co-director of the Consultative Service.
“Words cannot express the meaningful impact Dr. Mihm had on my career. Over the years, he became a close friend and a family member. He embodied the concept of true mentorship and friendship for life,” Piris said.
Colleagues and friends noted that Dr. Mihm always remained committed to helping others and acting as a positive influence in people’s lives.
“Up until the final days of his life, he was committed to helping others through his unparalleled kindness, knowledge and compassion,” Schatton said. “Martin’s warmth to everyone around him, without exception, made him a very rare individual, and his absence will be felt by many.”
Dr. Mihm is survived by his cousins, godchildren and loving friends.














 Once again, Brigham and Women’s Hospital has been recognized as a top hospital in the 2022 U.S. News & World Report’s annual ranking of the best U.S. hospitals. The Brigham was ranked 14th by the publication, while its Obstetrics & Gynecology specialty was named the best in the country — a noteworthy affirmation at a time when access to reproductive health services is being challenged across the U.S. In all, four specialties earned a spot in the top 10 and three specialties made the top five.
Once again, Brigham and Women’s Hospital has been recognized as a top hospital in the 2022 U.S. News & World Report’s annual ranking of the best U.S. hospitals. The Brigham was ranked 14th by the publication, while its Obstetrics & Gynecology specialty was named the best in the country — a noteworthy affirmation at a time when access to reproductive health services is being challenged across the U.S. In all, four specialties earned a spot in the top 10 and three specialties made the top five.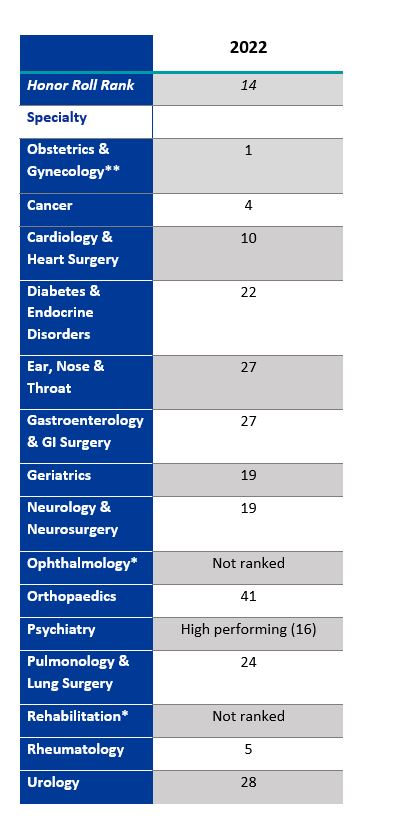
 Brigham and Women’s Hospital mourns the loss of Robert Osteen, MD, a cancer surgeon and educator whose contributions to the field of surgical oncology influenced generations of surgeons. He died July 14 from complications following a recent injury. He was 81.
Brigham and Women’s Hospital mourns the loss of Robert Osteen, MD, a cancer surgeon and educator whose contributions to the field of surgical oncology influenced generations of surgeons. He died July 14 from complications following a recent injury. He was 81. Brigham and Women’s Hospital mourns the loss of Sunni Reis, BSN, RN, a nurse in the Emergency Department (ED), who passed away June 7. She was 37.
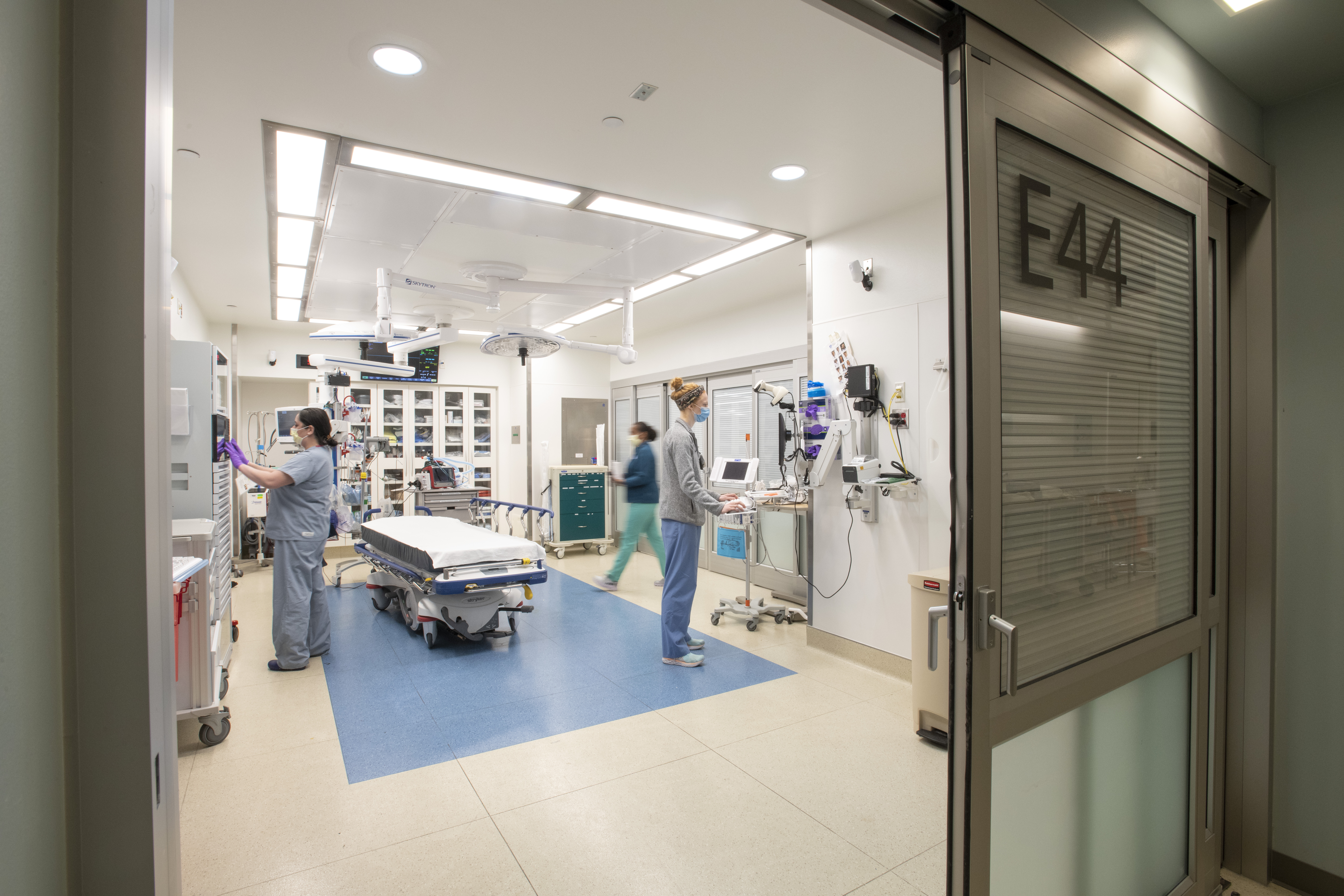
Brigham and Women’s Hospital mourns the loss of Sunni Reis, BSN, RN, a nurse in the Emergency Department (ED), who passed away June 7. She was 37.



















 Shaina A. Lipa, MD, MPH
Shaina A. Lipa, MD, MPH Gezzer Ortega, MD, MPH
Gezzer Ortega, MD, MPH

























 Over the past few years, numerous departments across the Brigham have stepped up to continuously meet arising challenges in our community, and the Police, Security and Commuter Services department has been no exception.
Over the past few years, numerous departments across the Brigham have stepped up to continuously meet arising challenges in our community, and the Police, Security and Commuter Services department has been no exception. “We provide safety planning, so if an employee feels threatened or unsafe, they can sit down with our community service officers and design personalized safety plans,” noted Slattery.
“We provide safety planning, so if an employee feels threatened or unsafe, they can sit down with our community service officers and design personalized safety plans,” noted Slattery.
 All are welcome to share condolences and memories of Dr. Welch in the comments section below the story.
All are welcome to share condolences and memories of Dr. Welch in the comments section below the story. All are welcome to share condolences and memories of Mr. Radhakrishna in the comments section below the story.
All are welcome to share condolences and memories of Mr. Radhakrishna in the comments section below the story. Surveyors from The Joint Commission (TJC) are expected to visit the Brigham unannounced to conduct BWH’s triennial, hospital-wide accreditation survey any day now. Our goal during the five-day visit is to demonstrate the unwavering commitment we have to our staff, patients and their families, our dedication to upholding the highest standards of quality and safety and our work to ensure that our practices are consistent with the
Surveyors from The Joint Commission (TJC) are expected to visit the Brigham unannounced to conduct BWH’s triennial, hospital-wide accreditation survey any day now. Our goal during the five-day visit is to demonstrate the unwavering commitment we have to our staff, patients and their families, our dedication to upholding the highest standards of quality and safety and our work to ensure that our practices are consistent with the  V-Day is a globally-organized response against violence towards all women. Each year on V-Day, events take place worldwide to raise awareness about marginalized communities experiencing IPV. This year, the Brigham Medicine Grand Rounds examined IPV experienced by people of all gender identities and sexual orientations. Survivors and advocates were invited to share their stories and discuss how healthcare professionals can better identify and care for victims of IPV in medical settings.
V-Day is a globally-organized response against violence towards all women. Each year on V-Day, events take place worldwide to raise awareness about marginalized communities experiencing IPV. This year, the Brigham Medicine Grand Rounds examined IPV experienced by people of all gender identities and sexual orientations. Survivors and advocates were invited to share their stories and discuss how healthcare professionals can better identify and care for victims of IPV in medical settings.


 For Margaret Hayden, MD, and Sanjay Kishore, MD, working exceptionally long hours as medical residents is far easier when together.
For Margaret Hayden, MD, and Sanjay Kishore, MD, working exceptionally long hours as medical residents is far easier when together. For many high school students, navigating future career options can feel daunting. But for Musarat Tasmin, the Brigham’s Student Success Jobs Program (SSJP) has illuminated research careers she never knew existed and provided her the mentorship needed to seek those opportunities.
For many high school students, navigating future career options can feel daunting. But for Musarat Tasmin, the Brigham’s Student Success Jobs Program (SSJP) has illuminated research careers she never knew existed and provided her the mentorship needed to seek those opportunities. For Yilu Ma, MS, MA, CMI, director of Interpreter Services, SSJP is not just about teaching students the skills they need to succeed in the workforce, but also helping them identify how to pursue their ambitions.
For Yilu Ma, MS, MA, CMI, director of Interpreter Services, SSJP is not just about teaching students the skills they need to succeed in the workforce, but also helping them identify how to pursue their ambitions.
 Small acts of kindness can make a tremendous difference in our workplace, especially during challenging times.
Small acts of kindness can make a tremendous difference in our workplace, especially during challenging times.  Chadwick Balcom began her card-making endeavors by sending cards to family, friends and colleagues. She spread the word through her Facebook network, a dedicated card-making Instagram account (heart2handmadecards) and
Chadwick Balcom began her card-making endeavors by sending cards to family, friends and colleagues. She spread the word through her Facebook network, a dedicated card-making Instagram account (heart2handmadecards) and  Kayla Pedersen, BSN, RN, a nurse on Braunwald Tower 8CD, understands very well the impact of kindness and compassion. While caring for a patient transitioning to comfort measures only, she handed him a piece of paper and asked him what he would like to say to his wife. He wrote, “I love you forever.” Pedersen matted and framed the handwritten message, placing it on his bedside table. His words of eternal love were the first thing his wife saw upon arriving the next day during such a heart-wrenching time.
Kayla Pedersen, BSN, RN, a nurse on Braunwald Tower 8CD, understands very well the impact of kindness and compassion. While caring for a patient transitioning to comfort measures only, she handed him a piece of paper and asked him what he would like to say to his wife. He wrote, “I love you forever.” Pedersen matted and framed the handwritten message, placing it on his bedside table. His words of eternal love were the first thing his wife saw upon arriving the next day during such a heart-wrenching time. With cold temperatures and frost settling in, there’s no mistaking that winter is here. For many, staying warm this season means staying inside. And coming off the holiday months — a time often spent with loved ones, indulging in sweet treats and generations-old recipes — individuals can find it challenging to maintain regular wellness routines.
With cold temperatures and frost settling in, there’s no mistaking that winter is here. For many, staying warm this season means staying inside. And coming off the holiday months — a time often spent with loved ones, indulging in sweet treats and generations-old recipes — individuals can find it challenging to maintain regular wellness routines.  Florina Haimovici, MD, director of the Brigham’s Reproductive Endocrinology and Infertility Psychiatric Clinic and a psychiatrist with Brigham and Women’s Faulkner Hospital’s Consultation Liaison Service, smiled, wiping a tear from her eye as she reflected on how much the Brigham community meant to her and her family.
Florina Haimovici, MD, director of the Brigham’s Reproductive Endocrinology and Infertility Psychiatric Clinic and a psychiatrist with Brigham and Women’s Faulkner Hospital’s Consultation Liaison Service, smiled, wiping a tear from her eye as she reflected on how much the Brigham community meant to her and her family. In May, Haimovici’s husband received a phone call from the Brigham’s kidney donor practice manager, letting him know that they had identified a donor. The donor was a perfect match and the practice manager asked Haimovici and Iancovici if they would like to know the donor.
In May, Haimovici’s husband received a phone call from the Brigham’s kidney donor practice manager, letting him know that they had identified a donor. The donor was a perfect match and the practice manager asked Haimovici and Iancovici if they would like to know the donor. Haimovici spoke of the unconditional support she received from her colleagues throughout this journey. She said she could not have made it through this process without the backing of her department.
Haimovici spoke of the unconditional support she received from her colleagues throughout this journey. She said she could not have made it through this process without the backing of her department. Behind the bustling clinical operations on the frontlines of hospital management is a small yet integral support team the Brigham depends on to run every day. That’s the Linen Department.
Behind the bustling clinical operations on the frontlines of hospital management is a small yet integral support team the Brigham depends on to run every day. That’s the Linen Department.

