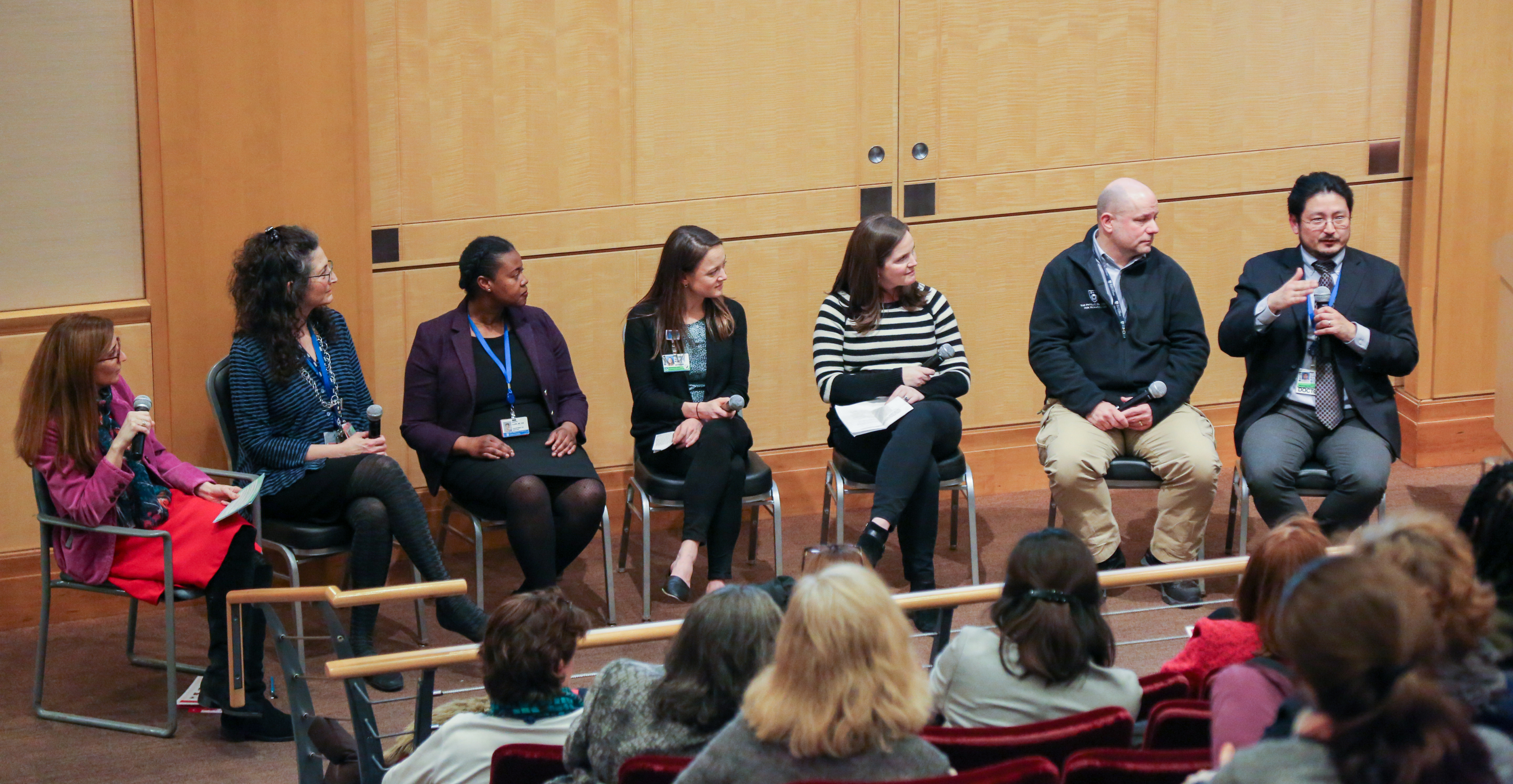Safe Care Commitment Spotlight: Expanded COVID-19 Testing Team
The Brigham’s Safe Care Commitment assures patients that We Screen, We Clean and We Protect. We are grateful to all staff who are working to demonstrate this commitment to our patients. If you know someone who exemplifies this commitment, please nominate them to be featured in our Safe Care Commitment Spotlight by emailing bulletin@bwh.harvard.edu with a few sentences about why you are nominating them.
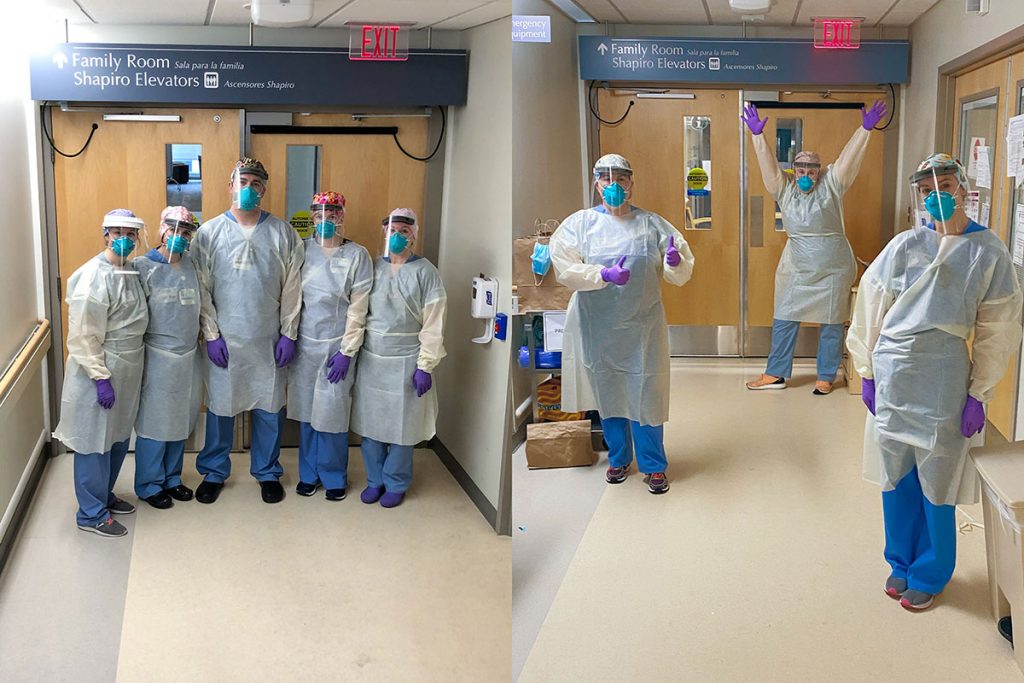
Today we are featuring the Expanded COVID-19 Testing team. Within 24 hours of an initial phone call with leaders at the Brigham, Broad Institute and the Cambridge Innovation Center, the hospital had an employee testing site up and running on Sept. 25. Since the site opened, the team has tested over 7,000 employees and received over 6,000 results.
Eric Goralnick, MD, MS, medical director of Emergency Preparedness and the Access Center, was struck by the determination, focus and can-do attitude of the testing site’s interdisciplinary team, led by Paula Kackley, MBA, executive director of Brigham Clinical Services and interim executive director of Operations, Mass General Brigham Urgent Care, and Susannah Rudel, MBA, MPH, Deland Fellow.
“This team really exemplifies the Brigham Way: identifying a new challenge and teaming on solutions to best care for each other within our community,” Goralnick said.
Kelly O’Connell, PA-C, an instructor and observer of the testing in Zinner, said she was happy to have the opportunity to be a part of the testing program.
“This initiative has offered a peace of mind to Brigham staff,” O’Connell said. “It has been rewarding to meet many colleagues and provide each of them with quick and convenient access to a test.”



































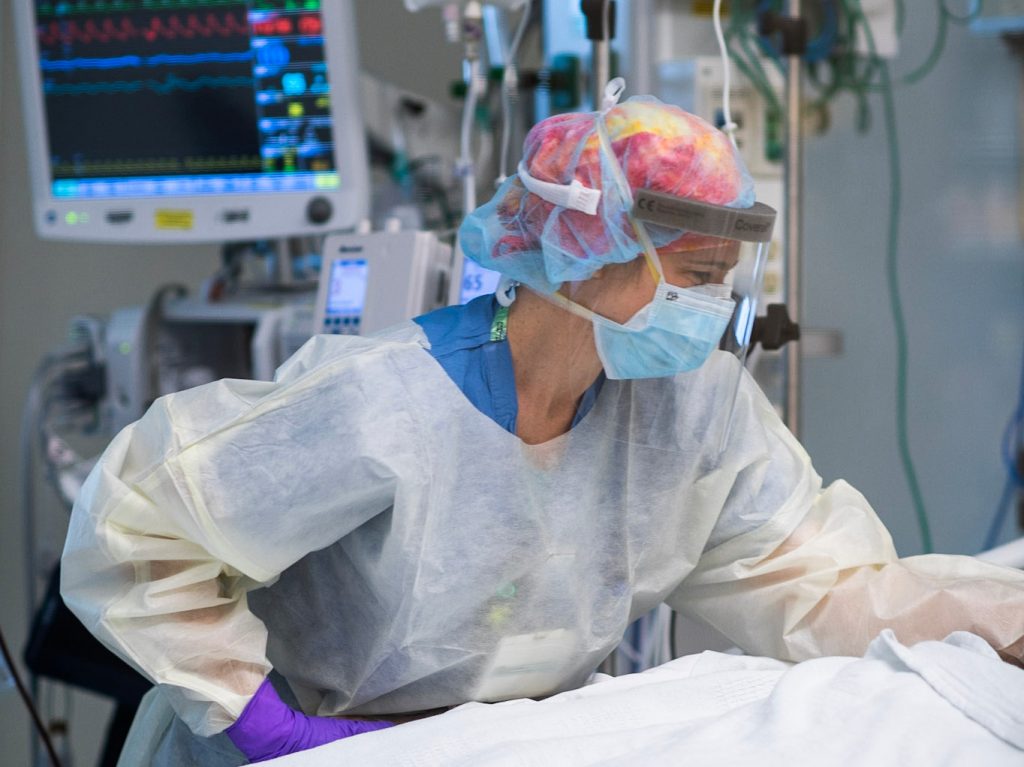


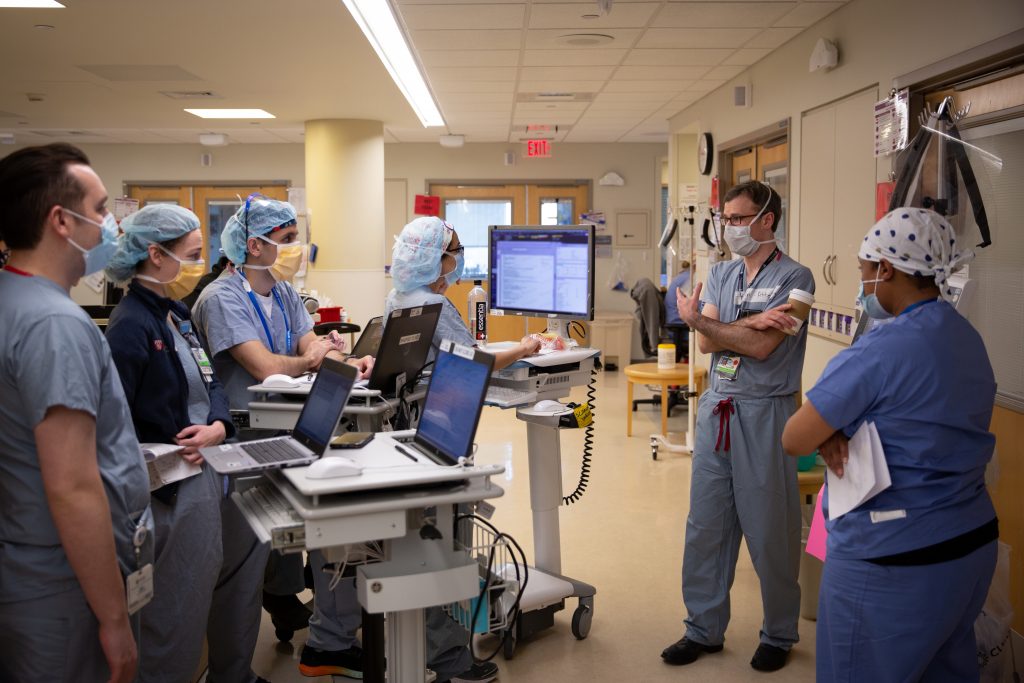


























 “COVID-19 has turned our world upside down. Our work, our homes, our spaces, our assumptions and how we spend our time have all fundamentally changed. But one thing that has not changed has been our commitment to one another. Our care, concern and kindnesses to one another have only increased during this pandemic. This has been what has sustained me throughout this pandemic and continues to inspire and strengthen me. Thank you to all.”
“COVID-19 has turned our world upside down. Our work, our homes, our spaces, our assumptions and how we spend our time have all fundamentally changed. But one thing that has not changed has been our commitment to one another. Our care, concern and kindnesses to one another have only increased during this pandemic. This has been what has sustained me throughout this pandemic and continues to inspire and strengthen me. Thank you to all.” “I will never forget the sense of enormity of the task that faced us in the early days of the pandemic in preparing to care for COVID-19 patients while controlling the spread of infection and keeping our staff safe. I will also remember the countless infection control-related challenges we encountered along the way, including PPE shortages, limited testing capacity, need for more airborne-infection isolation rooms, changing public health guidance and our incomplete but evolving knowledge of COVID-19 epidemiology and transmission. Most memorable, however, is the dedication, selflessness, comradery and shared sense of purpose I witnessed from the Incident Command team and the many other people involved in the hospital’s response.”
“I will never forget the sense of enormity of the task that faced us in the early days of the pandemic in preparing to care for COVID-19 patients while controlling the spread of infection and keeping our staff safe. I will also remember the countless infection control-related challenges we encountered along the way, including PPE shortages, limited testing capacity, need for more airborne-infection isolation rooms, changing public health guidance and our incomplete but evolving knowledge of COVID-19 epidemiology and transmission. Most memorable, however, is the dedication, selflessness, comradery and shared sense of purpose I witnessed from the Incident Command team and the many other people involved in the hospital’s response.”

















 Launching Monday, March 9, the Brigham Experience: Employee Engagement Survey will invite all Brigham Health staff to provide confidential feedback about our workplace and culture.
Launching Monday, March 9, the Brigham Experience: Employee Engagement Survey will invite all Brigham Health staff to provide confidential feedback about our workplace and culture.