A Special Shoutout to 221 Longwood Security and Parking Staff
As the Practice Manager in the Center for Child Development at 221 Longwood, I’d like to share how amazing our security and parking team members are.
Despite an incredibly challenging year, I am warmly greeted by Marilyn, our security guard, every single day. Her positivity continues to give me a reason to smile. Everyone who supports 221 is incredible, and I feel lucky to come to work every day.
I often think about how our patients’ care experiences begin when they pull up to 221 Longwood Ave, and as such, I consider our parking and security staff to be invaluable members of our team. I am so thankful to work alongside a fantastic group of individuals.
There is something very special in the air at 221 Longwood.
Kristen Sullivan
Practice Manager, Center for Child Development

 During the first surge of COVID-19, my hard work was rewarded when I was selected to go to see the New England Patriots game in Florida. I got to fly in the Patriots’ private plane then watch their game. It was the experience of a lifetime, and a moment I will cherish forever.
During the first surge of COVID-19, my hard work was rewarded when I was selected to go to see the New England Patriots game in Florida. I got to fly in the Patriots’ private plane then watch their game. It was the experience of a lifetime, and a moment I will cherish forever.  This year, we were honored to partner with SOAR Natick to sponsor their exhibit of 2,104 purple flags on the Stoneman Centennial Park to recognize National Recovery Month. Each flag represented someone who died from an opioid overdose in Massachusetts in the prior year. Several people from the hospital helped put up the exhibit, which was both heartbreaking and inspirational. The heartbreak was obvious: every flag we put up represented someone from our small state who had their life needlessly taken because of opioid overdose. These flags eventually covered most of the lawn to create a sea of purple: the color of recovery. The inspiration came from so many members of the community and hospital who came together not only to put up the exhibit, but to renew their commitment towards helping individuals struggling with opioid use disorder.
This year, we were honored to partner with SOAR Natick to sponsor their exhibit of 2,104 purple flags on the Stoneman Centennial Park to recognize National Recovery Month. Each flag represented someone who died from an opioid overdose in Massachusetts in the prior year. Several people from the hospital helped put up the exhibit, which was both heartbreaking and inspirational. The heartbreak was obvious: every flag we put up represented someone from our small state who had their life needlessly taken because of opioid overdose. These flags eventually covered most of the lawn to create a sea of purple: the color of recovery. The inspiration came from so many members of the community and hospital who came together not only to put up the exhibit, but to renew their commitment towards helping individuals struggling with opioid use disorder.  Earlier this year, I had the opportunity to engage in deep conversations with nurses and interprofessional colleagues about the pandemic, stress and self-care for our podcast series on resilience. I learned so much from the wisdom and compassion that my colleagues shared when reflecting on their experiences coping with stress. I reflect on those conversations often and draw on the lessons that I learned from this incredible group of people. To properly care for our patients, we must first take care of ourselves and each other. I’m proud to be part of such a thoughtful and supportive community during these challenging times.
Earlier this year, I had the opportunity to engage in deep conversations with nurses and interprofessional colleagues about the pandemic, stress and self-care for our podcast series on resilience. I learned so much from the wisdom and compassion that my colleagues shared when reflecting on their experiences coping with stress. I reflect on those conversations often and draw on the lessons that I learned from this incredible group of people. To properly care for our patients, we must first take care of ourselves and each other. I’m proud to be part of such a thoughtful and supportive community during these challenging times. I am so grateful to have assisted with putting together the Gratitude and Wellness Wall for staff. This interactive display on the Pike was a sacred place where we could all share self-care tips and how we have been making our days brighter during this difficult time. Seeing the wall fill with responses made my heart feel so full. I was proud to represent the Brigham community as I shared the story behind the wall on an episode of Chronicle.
I am so grateful to have assisted with putting together the Gratitude and Wellness Wall for staff. This interactive display on the Pike was a sacred place where we could all share self-care tips and how we have been making our days brighter during this difficult time. Seeing the wall fill with responses made my heart feel so full. I was proud to represent the Brigham community as I shared the story behind the wall on an episode of Chronicle.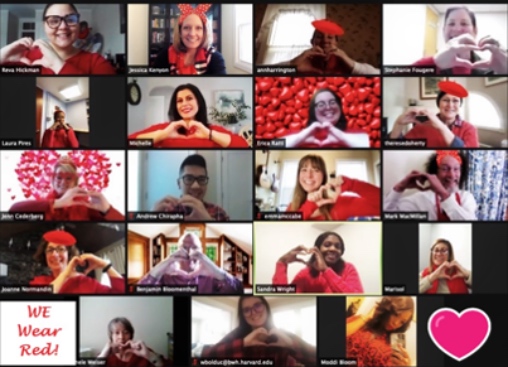 When an administrative team in cardiovascular medicine comes together to recognize women suffering from heart disease, it’s a beautiful and very proud moment for everyone involved. We were featured on e-boards throughout the hospital and continue to take great pride in our faculty’s efforts to improve the lives of others. Kudos to our then administrator, Jessica Kenyon, now executive director of the Department of Neurology, for inspiring us to come together to support our patients, each other, the American Heart Association and women nationwide.
When an administrative team in cardiovascular medicine comes together to recognize women suffering from heart disease, it’s a beautiful and very proud moment for everyone involved. We were featured on e-boards throughout the hospital and continue to take great pride in our faculty’s efforts to improve the lives of others. Kudos to our then administrator, Jessica Kenyon, now executive director of the Department of Neurology, for inspiring us to come together to support our patients, each other, the American Heart Association and women nationwide. “Interpreter Services does it again!”
“Interpreter Services does it again!”  Upon arriving at the Brigham, the first person to greet me was John Nyonnoh at the 15 Francis security desk. He stood, gave me a warm handshake and made me feel so welcome. He even told me about his family and showed me photos. His greeting reinstated everything I had heard about the Brigham: that everyone here is a family. This encounter made me feel incredibly lucky to be here. I’m immensely grateful that our patients, visitors, faculty and staff have such a terrific ambassador in John looking out for them.
Upon arriving at the Brigham, the first person to greet me was John Nyonnoh at the 15 Francis security desk. He stood, gave me a warm handshake and made me feel so welcome. He even told me about his family and showed me photos. His greeting reinstated everything I had heard about the Brigham: that everyone here is a family. This encounter made me feel incredibly lucky to be here. I’m immensely grateful that our patients, visitors, faculty and staff have such a terrific ambassador in John looking out for them. One of my favorite moments from the past year was this fall’s employee recognition event, where staff had the opportunity to directly connect with and support our community organizations. We offered fall-themed treats to employees across the Brigham, who helped pay our thanks forward by casting their vote for one of three local, non-profit organizations to receive a $10,000 charitable donation from the Brigham in appreciation of their partnership. We were thrilled to select the Immigrant Family Services Institute (IFSI), an organization dedicated to supporting recent immigrants’ integration into the United States’ social and economic systems. We were also glad to provide $5,000 contributions to the runners-up, City Life/Vida Urbana and Mattapan Food & Fitness Coalition. Regardless of the organizations chosen, I hope that this event strengthened our connections to the communities we serve.
One of my favorite moments from the past year was this fall’s employee recognition event, where staff had the opportunity to directly connect with and support our community organizations. We offered fall-themed treats to employees across the Brigham, who helped pay our thanks forward by casting their vote for one of three local, non-profit organizations to receive a $10,000 charitable donation from the Brigham in appreciation of their partnership. We were thrilled to select the Immigrant Family Services Institute (IFSI), an organization dedicated to supporting recent immigrants’ integration into the United States’ social and economic systems. We were also glad to provide $5,000 contributions to the runners-up, City Life/Vida Urbana and Mattapan Food & Fitness Coalition. Regardless of the organizations chosen, I hope that this event strengthened our connections to the communities we serve. I am a proud member of the Brigham’s thriving Physician Assistant (PA) community. In the last two years, I have been floored by our collective devotion to patients, academia and one another during the trying times that the COVID-19 pandemic has led. We’ve observed no shortage of clinicians going above and beyond during this period, but my most heartfelt moments have been amongst my colleagues, the PAs. Spanning across every medical specialty, I’ve witnessed PAs dedicating themselves to COVID-19 education in preparation to cross-cover areas in most need during the surge. As we enter yet another wave of COVID-19 with the Omicron variant, I have no doubt of our advanced team’s capabilities. It has been an honor to work alongside such incredible humans with a shared commitment to exceptional, selfless and equal care for all, a mission we all stand behind.
I am a proud member of the Brigham’s thriving Physician Assistant (PA) community. In the last two years, I have been floored by our collective devotion to patients, academia and one another during the trying times that the COVID-19 pandemic has led. We’ve observed no shortage of clinicians going above and beyond during this period, but my most heartfelt moments have been amongst my colleagues, the PAs. Spanning across every medical specialty, I’ve witnessed PAs dedicating themselves to COVID-19 education in preparation to cross-cover areas in most need during the surge. As we enter yet another wave of COVID-19 with the Omicron variant, I have no doubt of our advanced team’s capabilities. It has been an honor to work alongside such incredible humans with a shared commitment to exceptional, selfless and equal care for all, a mission we all stand behind. This past year was so challenging for so many. Brookside hosted COVID-19 testing and vaccine clinics and did our best to support our teams and meet our patients’ healthcare needs. We also wanted to recognize that in the midst of it all, Brookside turned 50! We celebrated by hiring an artist, Laura DeDonato, to create a mural that reflects who we are and who we’re becoming. Our staff created a vision through a few brainstorming sessions, and Laura made it all come to life. It was an exhausting year for all, but one that brought us closer together. As always, a shout-out to the Brookside team for being the best!
This past year was so challenging for so many. Brookside hosted COVID-19 testing and vaccine clinics and did our best to support our teams and meet our patients’ healthcare needs. We also wanted to recognize that in the midst of it all, Brookside turned 50! We celebrated by hiring an artist, Laura DeDonato, to create a mural that reflects who we are and who we’re becoming. Our staff created a vision through a few brainstorming sessions, and Laura made it all come to life. It was an exhausting year for all, but one that brought us closer together. As always, a shout-out to the Brookside team for being the best! On Dec. 1, we welcomed Robert Higgins, MD, MSHA, as the new Brigham president and the executive vice president of Mass General Brigham.
On Dec. 1, we welcomed Robert Higgins, MD, MSHA, as the new Brigham president and the executive vice president of Mass General Brigham. 
 Allen was immediately airlifted to the Brigham, where he would remain for 40 nights. After landing, doctors quickly decided Allen needed to go on ECMO, a form of life support for patients facing respiratory failure. Doing this, however, required his family’s consent and Allen’s family could not be found.
Allen was immediately airlifted to the Brigham, where he would remain for 40 nights. After landing, doctors quickly decided Allen needed to go on ECMO, a form of life support for patients facing respiratory failure. Doing this, however, required his family’s consent and Allen’s family could not be found. On Dec. 6, the Brigham’s
On Dec. 6, the Brigham’s 

 Do you have a memory from the past year that made you proud to be a part of our Brigham community?
Do you have a memory from the past year that made you proud to be a part of our Brigham community? Joseph Thibodeau is no stranger to adversity. After overcoming stage four lymphoma, battling graft-versus-host disease and later, having both his legs amputated due to an infection, Thibodeau has discovered firsthand the value of resilience.
Joseph Thibodeau is no stranger to adversity. After overcoming stage four lymphoma, battling graft-versus-host disease and later, having both his legs amputated due to an infection, Thibodeau has discovered firsthand the value of resilience. Last week, the Brigham community joined festivities grounded in gratitude and kindness. Employees across our main and distributed campus locations enjoyed fall-themed treats and helped pay our thanks forward by casting their vote for one of three local, non-profit organizations to receive a $10,000 charitable donation from the Brigham in appreciation of their partnership.
Last week, the Brigham community joined festivities grounded in gratitude and kindness. Employees across our main and distributed campus locations enjoyed fall-themed treats and helped pay our thanks forward by casting their vote for one of three local, non-profit organizations to receive a $10,000 charitable donation from the Brigham in appreciation of their partnership. While doing some gardening in their backyard earlier this year, Yazmine, 30, turned to her partner, Mayron, 25, with an idea about their upcoming wedding.
While doing some gardening in their backyard earlier this year, Yazmine, 30, turned to her partner, Mayron, 25, with an idea about their upcoming wedding. “Our compassionate Labor and Delivery staff quickly brought the idea to my attention of having their wedding on the L&D unit prior to the unexpectedly early birth of their baby,” she said. “The staff were thrilled and excited to help facilitate their wedding ceremony. The joy this sort of event brings to everyone working is tremendous. We are accustomed to the joys of childbirth, but to add a wedding to our day is extra special.”
“Our compassionate Labor and Delivery staff quickly brought the idea to my attention of having their wedding on the L&D unit prior to the unexpectedly early birth of their baby,” she said. “The staff were thrilled and excited to help facilitate their wedding ceremony. The joy this sort of event brings to everyone working is tremendous. We are accustomed to the joys of childbirth, but to add a wedding to our day is extra special.” Maureen Zuzevich, recruitment program manager for the Kraft Family Blood Donor Center, was heading home last year from a blood drive she had coordinated at Gillette Stadium when she was overcome by nausea. She quickly pulled over to the side of the road.
Maureen Zuzevich, recruitment program manager for the Kraft Family Blood Donor Center, was heading home last year from a blood drive she had coordinated at Gillette Stadium when she was overcome by nausea. She quickly pulled over to the side of the road.
































 Brigham and Women’s Hospital earned a spot once again on U.S. News & World Report’s list of Best Hospitals, being named No. 14 on the magazine’s 2021 Honor Roll rankings. The Honor Roll is a distinction awarded to 20 hospitals in the country that deliver the best care for the most serious or complicated medical conditions and procedures.
Brigham and Women’s Hospital earned a spot once again on U.S. News & World Report’s list of Best Hospitals, being named No. 14 on the magazine’s 2021 Honor Roll rankings. The Honor Roll is a distinction awarded to 20 hospitals in the country that deliver the best care for the most serious or complicated medical conditions and procedures.