Brigham Team Recognized for Role in Disaster Response
 When a major flood caused by a burst pipe forced the closure of the labor and delivery and neonatal intensive care units at Boston Medical Center (BMC) temporarily last year, the Brigham and several other hospitals stepped up to ensure patient care remained the priority.
When a major flood caused by a burst pipe forced the closure of the labor and delivery and neonatal intensive care units at Boston Medical Center (BMC) temporarily last year, the Brigham and several other hospitals stepped up to ensure patient care remained the priority.
During a Quality Rounds presentation in Bornstein Amphitheater last month, BMC clinicians spoke about the flood and reflected on the disaster response and lessons learned.
A critical piece to the emergency plan for BMC was the safe and timely transfer of patients out of the affected units to area hospitals, including the Brigham, for care. At the end of Quality Rounds, the Brigham was presented with an award from BMC in recognition of the assistance staff provided during the flood incident.
Karen Fiumara, PharmD, BCPS, executive director of Patient Safety at Brigham Health, said the Brigham teams that responded to this challenging situation were “nothing short of remarkable.”
“While continuing to safely care for their existing patients, they welcomed this group of BMC patients and their loved ones to the Brigham with open arms and provided them with exceptional care,” Fiumara said. “This was one of those amazing stories that makes you proud to be part of the Brigham community.”
Katherine Gregory, PhD, RN, associate chief nursing officer for the Mary Horrigan Connors Center for Women and Newborns, echoed Fiumara’s thoughts.
“The Brigham comes together in a crisis like no other, and we care—not only about our patients but also those across the city and region,” she said. “It was our privilege to care for the women and newborns who were affected by the BMC flood last year, and we stand ready to serve if called upon by our obstetric and newborn colleagues again in the future.”





 By far, my shining moment this year was the day I reconnected with my primary nurse, Vivian Kelley, RN, after 39 years! Vivian helped save my life back in 1979, when I came to the Peter Bent Brigham Hospital for a bone marrow transplant. I had aplastic anemia (a rare and life-threatening blood disease) and spent two and a half months in an isolation room. Vivian was there at every turn—when I got my chemo and during the hundreds of hours that followed as I waited for my new immune system to mature. The photo in which I’m wearing a mask marks the day I went home. The other picture was taken when we reconnected this summer in Boston. Vivian moved to the West Coast a year after my transplant and continued practicing nursing until she retired. I credit Vivian’s intelligence, nursing skills and her calm, positive attitude for getting me through a terrifying time in my life. I’m so grateful we found each other again.
By far, my shining moment this year was the day I reconnected with my primary nurse, Vivian Kelley, RN, after 39 years! Vivian helped save my life back in 1979, when I came to the Peter Bent Brigham Hospital for a bone marrow transplant. I had aplastic anemia (a rare and life-threatening blood disease) and spent two and a half months in an isolation room. Vivian was there at every turn—when I got my chemo and during the hundreds of hours that followed as I waited for my new immune system to mature. The photo in which I’m wearing a mask marks the day I went home. The other picture was taken when we reconnected this summer in Boston. Vivian moved to the West Coast a year after my transplant and continued practicing nursing until she retired. I credit Vivian’s intelligence, nursing skills and her calm, positive attitude for getting me through a terrifying time in my life. I’m so grateful we found each other again.



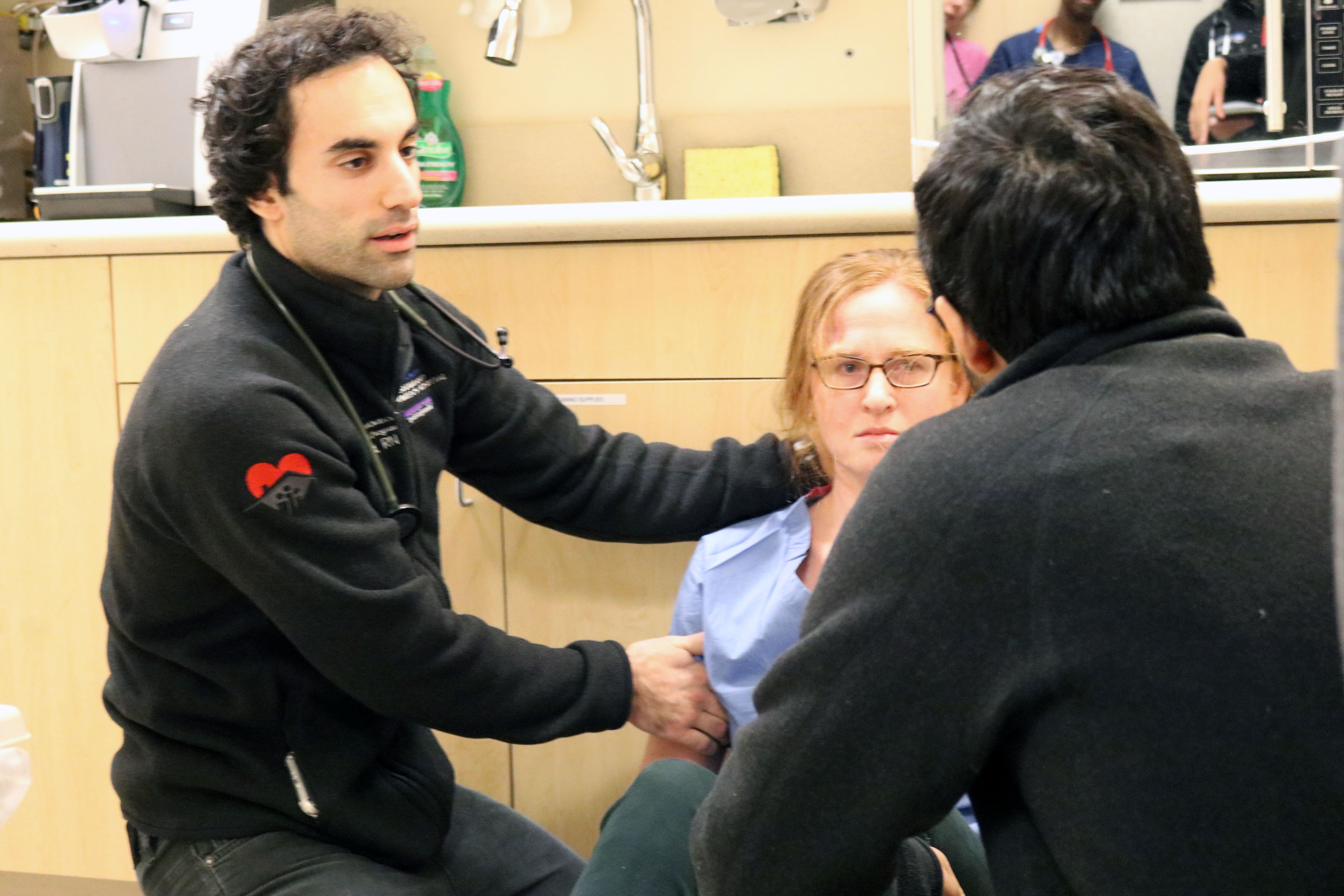

 “When I got that diagnosis, it hit me like a brick. I thought, wow, there’s something else going on,” she said. “Genetically speaking, there’s no explanation for it.”
“When I got that diagnosis, it hit me like a brick. I thought, wow, there’s something else going on,” she said. “Genetically speaking, there’s no explanation for it.”


 Staff from the Brigham’s Lung Center gathered for a celebratory breakfast on Oct. 29 before welcoming the first patients in their new clinic space on the Pike. The eight exam rooms and additional flex space enables the Lung Center’s three major disciplines – Pulmonary and Critical Care Medicine, Thoracic Surgery and Thoracic Oncology – to provide comprehensive, interdisciplinary care for patients in a single location. The clinic is located between the 15 Francis St. and 45 Francis St. entrances.
Staff from the Brigham’s Lung Center gathered for a celebratory breakfast on Oct. 29 before welcoming the first patients in their new clinic space on the Pike. The eight exam rooms and additional flex space enables the Lung Center’s three major disciplines – Pulmonary and Critical Care Medicine, Thoracic Surgery and Thoracic Oncology – to provide comprehensive, interdisciplinary care for patients in a single location. The clinic is located between the 15 Francis St. and 45 Francis St. entrances.




 ‘A Whole New Chapter’
‘A Whole New Chapter’











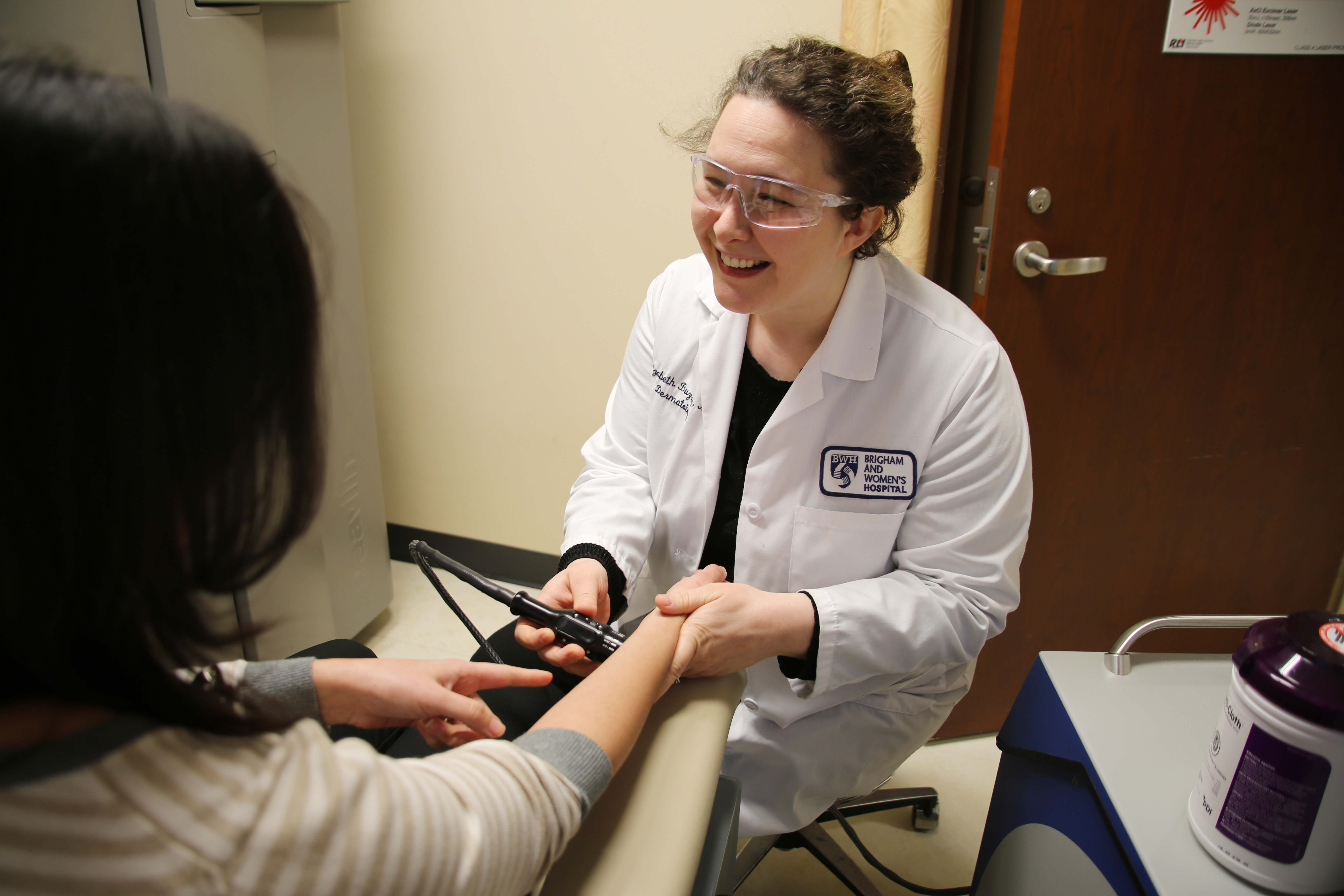











 One example of how these rounds led to improved care involved a patient with a serious brain injury who spent one year at the Brigham as an inpatient.
One example of how these rounds led to improved care involved a patient with a serious brain injury who spent one year at the Brigham as an inpatient.

 Massachusetts has been one of the states hit hardest by the nation’s opioid crisis, with the rate of opioid-related deaths seeing a fourfold increase between 2000 and 2015 across the state. In the span of just one year, 2013 to 2014, opioid-related deaths occurred in two-thirds of cities and towns in Massachusetts, according to the state Department of Public Health.
Massachusetts has been one of the states hit hardest by the nation’s opioid crisis, with the rate of opioid-related deaths seeing a fourfold increase between 2000 and 2015 across the state. In the span of just one year, 2013 to 2014, opioid-related deaths occurred in two-thirds of cities and towns in Massachusetts, according to the state Department of Public Health.
 “I didn’t think we were going to have enough hats, but then they poured in,” said Giller, who ultimately collected 550 hats, which are being distributed to infants in the Connors Center for Women and Newborns throughout February. “I am so grateful for every single hat that was made and for the people who helped spread the word. This would not be possible without everyone’s help.”
“I didn’t think we were going to have enough hats, but then they poured in,” said Giller, who ultimately collected 550 hats, which are being distributed to infants in the Connors Center for Women and Newborns throughout February. “I am so grateful for every single hat that was made and for the people who helped spread the word. This would not be possible without everyone’s help.”

 When the ED is at capacity, some patients leave after being seen by a triage nurse, but before being seen by a physician. When a “walkout” occurs – often due to long wait times – it not only leads to a poor patient experience, but it is also a safety concern, as nearly 30 percent of patients who receive care in the Brigham’s ED are sick enough to be admitted.
When the ED is at capacity, some patients leave after being seen by a triage nurse, but before being seen by a physician. When a “walkout” occurs – often due to long wait times – it not only leads to a poor patient experience, but it is also a safety concern, as nearly 30 percent of patients who receive care in the Brigham’s ED are sick enough to be admitted.


 Mohamed El-Dib, MD, director of Neonatal Critical Care in the Department of Pediatric Newborn Medicine, is the principal investigator at BWH for a multi-institutional clinical trial looking at whether infusing babies with their own umbilical cord blood can indeed reverse tissue damage in the brain.
Mohamed El-Dib, MD, director of Neonatal Critical Care in the Department of Pediatric Newborn Medicine, is the principal investigator at BWH for a multi-institutional clinical trial looking at whether infusing babies with their own umbilical cord blood can indeed reverse tissue damage in the brain.






