Happy New Year! Brigham Baby Marks a Precious Start to 2021

Left photo: Sarah and Benjamin Welch celebrate the birth of their daughter, Charlotte, on New Year’s Day; Right photo: Nurse Shayna Shaffer, RN, (far left) and obstetrician Carolyn Cline, MD, (far right) share a moment with the Welch family.
Baby Charlotte, weighing 8 pounds and 2 ounces, was one of the first babies born on New Year’s Day at the Brigham. Parents Sarah Welch, a senior physical therapist in Rehabilitation Services, and Benjamin Welch, welcomed their daughter into the world at 3:50 a.m.





 Amid the immense suffering and loss during the pandemic, we have witnessed beautiful examples of compassion and human connection in every setting. I was especially moved by how nurses at the bedside comforted dying patients who were otherwise alone, without loved ones present during their final moments.
Amid the immense suffering and loss during the pandemic, we have witnessed beautiful examples of compassion and human connection in every setting. I was especially moved by how nurses at the bedside comforted dying patients who were otherwise alone, without loved ones present during their final moments.

 Tengo 18 años trabajando para tan importante hospital como es el Mass General Brigham. He pasado por momentos difíciles, como las tormentas de nieve, donde a veces no podías llegar a la casa. Pero el más difícil es esta pandemia que nos ha tocado vivir, y a pesar de todo, seguimos fuertes y con una sonrisa de esperanza. Juntos somos fuertes. Feliz navidad. We are strong.
Tengo 18 años trabajando para tan importante hospital como es el Mass General Brigham. He pasado por momentos difíciles, como las tormentas de nieve, donde a veces no podías llegar a la casa. Pero el más difícil es esta pandemia que nos ha tocado vivir, y a pesar de todo, seguimos fuertes y con una sonrisa de esperanza. Juntos somos fuertes. Feliz navidad. We are strong.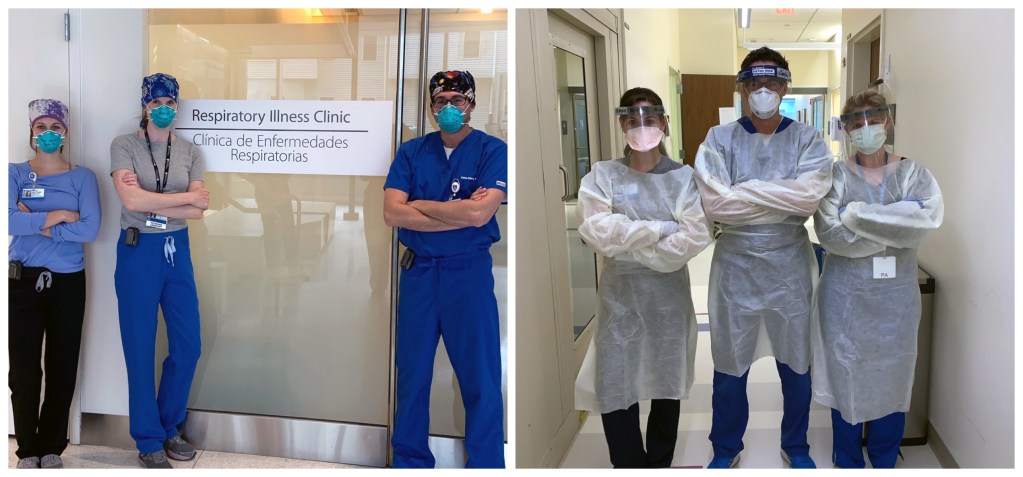

 The Operating Room (OR) facilitators are a team in the Operating Room who organize and maintain the OR desk. When the pandemic hit us hard in the spring, every one of them showed up to work every day, ready to help the team. With no questions asked, they were there to help others carry the load of the stressors everyone was facing. They are an integral part of the Operating Room who give 100 percent every day. The pride they take in their work is inspiring. They work together to strengthen the culture. I am continually impressed with their work ethic and results they produce.
The Operating Room (OR) facilitators are a team in the Operating Room who organize and maintain the OR desk. When the pandemic hit us hard in the spring, every one of them showed up to work every day, ready to help the team. With no questions asked, they were there to help others carry the load of the stressors everyone was facing. They are an integral part of the Operating Room who give 100 percent every day. The pride they take in their work is inspiring. They work together to strengthen the culture. I am continually impressed with their work ethic and results they produce.

 Shalaine Parker is a member of the Police and Security team who often plays the piano in the 45 Francis St. lobby while on break from her duties. I was there on a recent morning getting a coffee at Starbucks. It was a cold, gray November day, and when Shalaine sat down at the piano, I was startled by her incredible talent! Her music was beautiful and very soothing. I thanked her for brightening this dark day. I hope Shalaine is recognized for being a bright star at the Brigham!
Shalaine Parker is a member of the Police and Security team who often plays the piano in the 45 Francis St. lobby while on break from her duties. I was there on a recent morning getting a coffee at Starbucks. It was a cold, gray November day, and when Shalaine sat down at the piano, I was startled by her incredible talent! Her music was beautiful and very soothing. I thanked her for brightening this dark day. I hope Shalaine is recognized for being a bright star at the Brigham!
 Throughout the almost two and a half months I spent as a nurse on Shapiro 9 West, our first COVID-19 ICU, I met an angel named Lisa Beal. Lisa was an ICU extender and a fellow empathetic soul who helped create one shining moment for our patient.
Throughout the almost two and a half months I spent as a nurse on Shapiro 9 West, our first COVID-19 ICU, I met an angel named Lisa Beal. Lisa was an ICU extender and a fellow empathetic soul who helped create one shining moment for our patient.
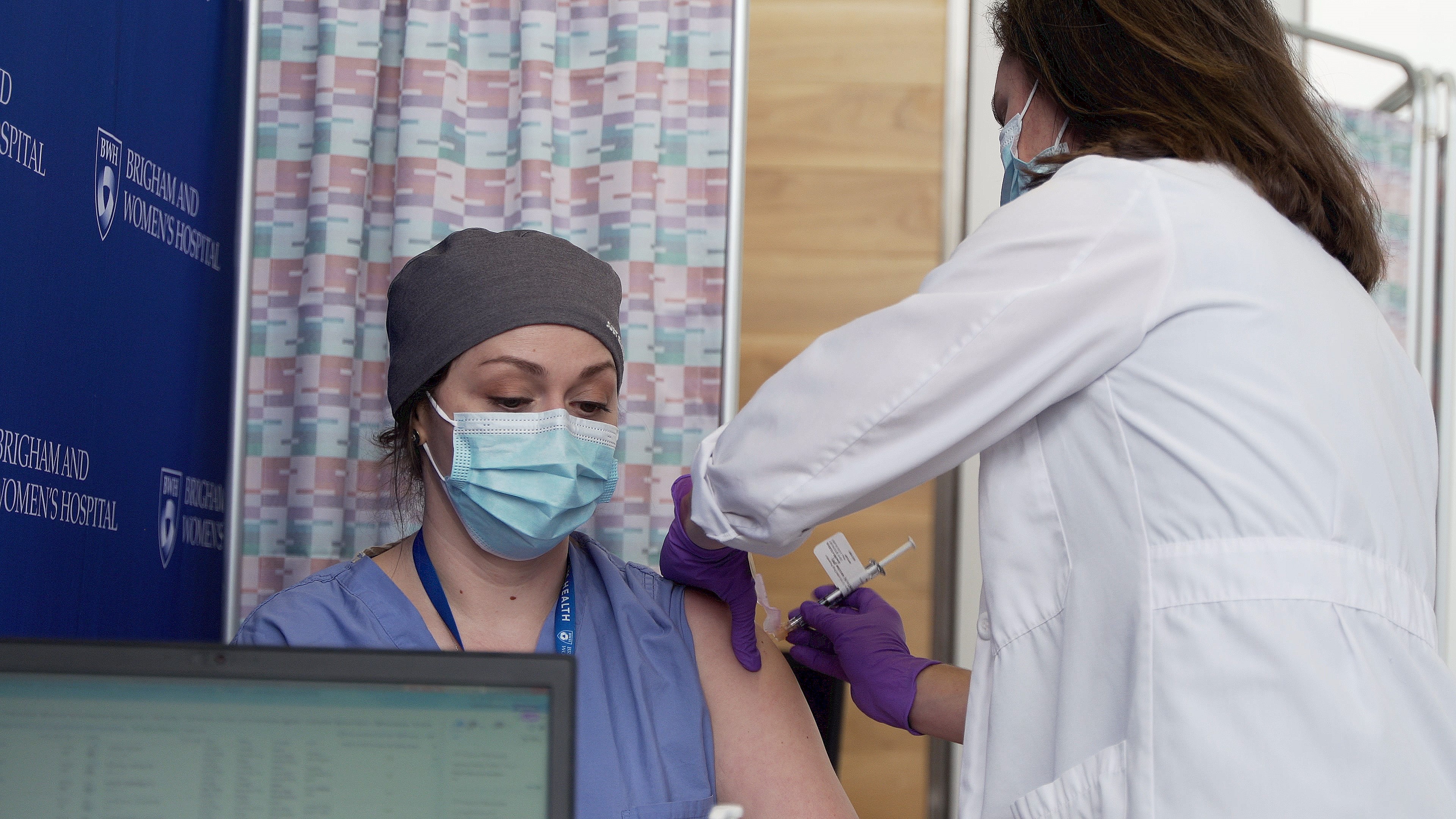
 “I feel very fortunate to be in a position to receive this vaccine. As we are in the midst of another surge, I just hope distribution can occur fast enough to decrease further illness and fatalities. I feel comfortable receiving the COVID-19 vaccine because I am confident in the endless efforts and commitment of all who participated in developing it.”
“I feel very fortunate to be in a position to receive this vaccine. As we are in the midst of another surge, I just hope distribution can occur fast enough to decrease further illness and fatalities. I feel comfortable receiving the COVID-19 vaccine because I am confident in the endless efforts and commitment of all who participated in developing it.” “If I believe it’s the right thing for society, then it’s the right thing for me and my family as well. I want to be beyond this epidemic as much as anybody else. I’m going on service later this month and will be taking care of COVID-positive patients, so I’m definitely looking forward to having this additional layer of protection.”
“If I believe it’s the right thing for society, then it’s the right thing for me and my family as well. I want to be beyond this epidemic as much as anybody else. I’m going on service later this month and will be taking care of COVID-positive patients, so I’m definitely looking forward to having this additional layer of protection.” “I watch the news every morning and read a lot of the articles. I believe the vaccine is very safe, and I want to be the first in line to get it! Working in Environmental Services, we have gone through a lot — especially at the beginning of the pandemic — and it’s been very hard. I want to feel safer coming to work. I know the vaccine has some secondary effects, but I prefer to deal with those mild symptoms at home one day than to get COVID and possibly be on a ventilator in the hospital.”
“I watch the news every morning and read a lot of the articles. I believe the vaccine is very safe, and I want to be the first in line to get it! Working in Environmental Services, we have gone through a lot — especially at the beginning of the pandemic — and it’s been very hard. I want to feel safer coming to work. I know the vaccine has some secondary effects, but I prefer to deal with those mild symptoms at home one day than to get COVID and possibly be on a ventilator in the hospital.” “I am very excited about starting the vaccines for all of our faculty and staff and view it as the ‘beginning of the end of the pandemic.’ Of course, I am also ready to get the vaccine personally as soon as I am eligible to receive it, based on Mass General Brigham (MGB) guidance. The FDA and CDC work and reporting, as well as our own Harvard and MGB review of the data, have given me confidence that the vaccine is safe and effective and made me ready to move forward. I don’t think I or others will feel completely comfortable until all of our families and friends can receive the vaccine, so we will have to remain careful and vigilant with our masking and distancing until that happens!”
“I am very excited about starting the vaccines for all of our faculty and staff and view it as the ‘beginning of the end of the pandemic.’ Of course, I am also ready to get the vaccine personally as soon as I am eligible to receive it, based on Mass General Brigham (MGB) guidance. The FDA and CDC work and reporting, as well as our own Harvard and MGB review of the data, have given me confidence that the vaccine is safe and effective and made me ready to move forward. I don’t think I or others will feel completely comfortable until all of our families and friends can receive the vaccine, so we will have to remain careful and vigilant with our masking and distancing until that happens!” “I have tremendous faith in the scientists, doctors, and public health officials who have helped create and facilitate the distribution of the COVID-19 vaccine. I look forward to being vaccinated for not only my own personal health but also for the health of my family, friends, patients and the wider community in which I interact. Vaccines are about population-wide health. In getting vaccinated for COVID-19, I will be proud to be part of a widespread effort to reinvigorate community-wide physical health, emotional well-being and economic vitality.”
“I have tremendous faith in the scientists, doctors, and public health officials who have helped create and facilitate the distribution of the COVID-19 vaccine. I look forward to being vaccinated for not only my own personal health but also for the health of my family, friends, patients and the wider community in which I interact. Vaccines are about population-wide health. In getting vaccinated for COVID-19, I will be proud to be part of a widespread effort to reinvigorate community-wide physical health, emotional well-being and economic vitality.” “I am excited and extremely comfortable getting the COVID-19 vaccine because I believe it will be reassuring for my primary care patients to know that their doctor has personally gotten the vaccine and advocates that they should as well. This is especially important for my older Vietnamese-American and Asian-American patients who may have a general distrust of vaccines to know that their Vietnamese-American doctor has received it. I also believe the vaccine will be another layer of protection for me against COVID-19.”
“I am excited and extremely comfortable getting the COVID-19 vaccine because I believe it will be reassuring for my primary care patients to know that their doctor has personally gotten the vaccine and advocates that they should as well. This is especially important for my older Vietnamese-American and Asian-American patients who may have a general distrust of vaccines to know that their Vietnamese-American doctor has received it. I also believe the vaccine will be another layer of protection for me against COVID-19.” “I plan to get vaccinated because I work with COVID-positive patients and need that extra protection. I was a little apprehensive at first, given it’s a new vaccine, but I feel that if the organization believes it’s safe for our physicians and other clinicians caring for our patients, then it must be safe. It feels good that we finally have something that offers hope of slowing or stopping this pandemic.”
“I plan to get vaccinated because I work with COVID-positive patients and need that extra protection. I was a little apprehensive at first, given it’s a new vaccine, but I feel that if the organization believes it’s safe for our physicians and other clinicians caring for our patients, then it must be safe. It feels good that we finally have something that offers hope of slowing or stopping this pandemic.” “I’m very excited and definitely plan on getting the vaccine when I’m able to. We’ve been in this pandemic for nine months, but somehow that nine months feels both like nine years and nine days. The current case numbers in our country have shown that social distancing and mask wearing isn’t enough. I believe that our way out of this pandemic and back to some form of normalcy is through a safe and effective vaccine. I’m excited that there’s a vaccine on the horizon and I’m excited for everyone and their communities to be able to receive it.”
“I’m very excited and definitely plan on getting the vaccine when I’m able to. We’ve been in this pandemic for nine months, but somehow that nine months feels both like nine years and nine days. The current case numbers in our country have shown that social distancing and mask wearing isn’t enough. I believe that our way out of this pandemic and back to some form of normalcy is through a safe and effective vaccine. I’m excited that there’s a vaccine on the horizon and I’m excited for everyone and their communities to be able to receive it.” “Like everyone, I’m relieved and elated that people will finally have access to a vaccine and I’m proud of the Brigham’s important role in getting us to this point. When it’s my turn (Wave D), I’ll be excited to get the vaccine. I’m also well aware that there’s still a lot of work to be done. Vaccine clinical trials are still underway, both to evaluate additional COVID vaccines and to continue the trials for the vaccines that have already been established. We still have a lot to learn about sustained immune response to COVID and these trials — and a number of other important research projects at the Brigham — will be critical to understanding that. We also continue to push the boundaries of diagnostic testing for COVID, both so that there will be a broader array of highly sensitive and specific testing tools accessible to as many people as possible and to provide the tools necessary to fully understand immune response to COVID.”
“Like everyone, I’m relieved and elated that people will finally have access to a vaccine and I’m proud of the Brigham’s important role in getting us to this point. When it’s my turn (Wave D), I’ll be excited to get the vaccine. I’m also well aware that there’s still a lot of work to be done. Vaccine clinical trials are still underway, both to evaluate additional COVID vaccines and to continue the trials for the vaccines that have already been established. We still have a lot to learn about sustained immune response to COVID and these trials — and a number of other important research projects at the Brigham — will be critical to understanding that. We also continue to push the boundaries of diagnostic testing for COVID, both so that there will be a broader array of highly sensitive and specific testing tools accessible to as many people as possible and to provide the tools necessary to fully understand immune response to COVID.” “I am looking forward to receiving the vaccine. Based on our knowledge about the virus and long-term effects, I am hopeful that this will help decrease the spread of the virus. The vaccine will help us from getting seriously ill even if we get the virus. I think the benefits of receiving the vaccine outweigh the risks of this virus.”
“I am looking forward to receiving the vaccine. Based on our knowledge about the virus and long-term effects, I am hopeful that this will help decrease the spread of the virus. The vaccine will help us from getting seriously ill even if we get the virus. I think the benefits of receiving the vaccine outweigh the risks of this virus.”