New COVID Recovery Center Seeks to Support ‘Long-Hauler’ Patients with Lingering Symptoms

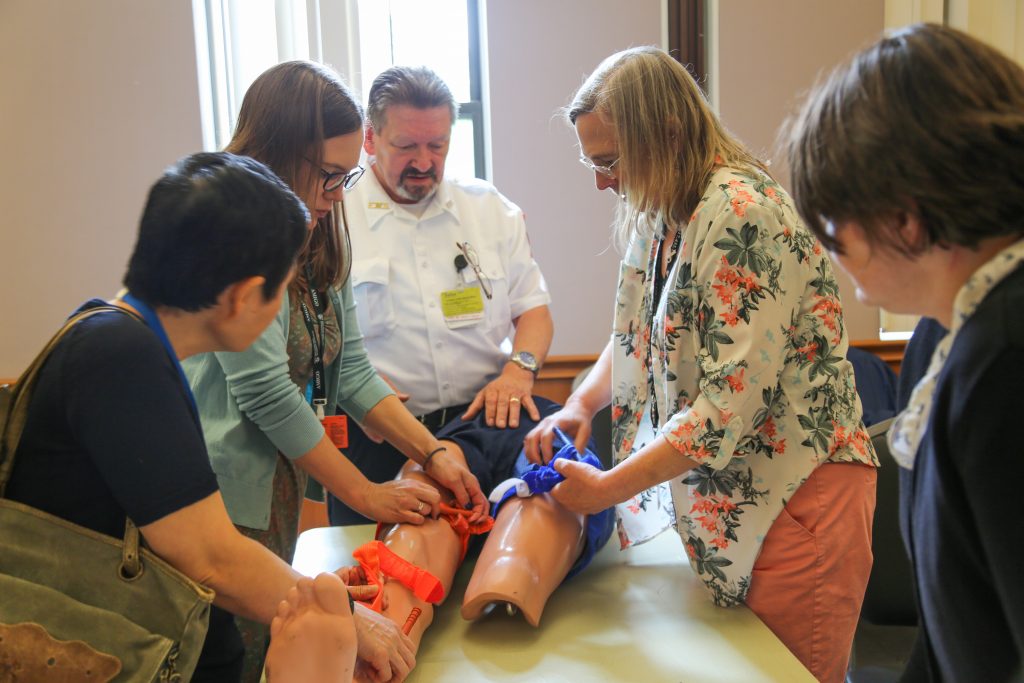
From left: Judy De Leon, medical assistant, Ann-Marcia Tukpah, clinical fellow in Pulmonology, and Fotine Liakopoulos, medical assistant, converse outside a patient room in the COVID Recovery Center, located in the Lung Center.
There were so many things Monique Vaughan, 31, used to do without a second thought.
She worked full-time, sometimes up to 60 hours per week, at a busy mental health facility. To clear her head after work, she took her dog on a leisurely walk through her neighborhood for 30 to 45 minutes. In college, she had taken courses to sharpen her IT skills, making it a breeze for her to troubleshoot technology issues at home.
All of that changed after Vaughan tested positive for COVID-19 over one year ago. Long after recovering from the initial infection — which made her sick enough to require hospitalization for several days — she continues to live with a variety of lingering symptoms that have significantly affected her quality of life. Over the past year, she has been coping with extreme fatigue, intense migraines, severe muscle pain and ongoing cognitive struggles (or “brain fog”) and memory loss.
As a result, Vaughan says she had to scale back her hours at work to part-time. Walking more than a block feels like running a marathon. Focusing on a seemingly basic task can feel impossible at times.
“I was recently having trouble with my router at home. I’m a millennial, so internet stuff has never been hard for me to figure out. It was an issue I had fixed many times before, but this time I couldn’t remember how to do it,” she said. “I got so frustrated that I just sat in front of the router and cried.”
Among the many concerning aspects of COVID-19 has been its long-term effects on the body and mind — a mystery that scientists and health care experts are still just beginning to understand.
Seeking to address the complex medical and psychosocial needs of “long-hauler” patients like Vaughan, the Brigham recently launched the COVID Recovery Center, a new clinical and research center that brings together experts from a diverse range of disciplines. Each patient is assigned a patient navigator to help coordinate their care and facilitate follow-up appointments, referrals and testing.
While located in the Brigham’s Lung Center, pulmonology is just one of the many specialties the center offers. Depending on what a patient’s individual needs are, they can also be connected with cardiologists, hematologists, infectious disease specialists, nephrologists, neurologists, psychiatrists, dietitians, social workers or other health care providers.
“A new illness mandates a new approach,” said Bruce Levy, MD, chief of the Division of Pulmonary and Critical Care Medicine. “A lot of the symptoms these patients are experiencing are rather non-specific, so primary care providers are often challenged to figure out who is best suited to help their post-COVID patient when help is needed. For patients who may be going to multiple specialty clinics, finding those locations and navigating that system is not easy either. In the COVID Recovery Center, our goal is to ensure COVID ‘long-hauler’ patients get the best, most efficient care possible.”
Centered on Collaboration and Equity
Collaboration is at the heart of the center’s strategy. A multidisciplinary team conducts weekly case reviews to ensure all aspects of a patient’s care plan are thoroughly evaluated. Similar centers recently established at Massachusetts General Hospital and the Spaulding Rehabilitation Hospital for recovering COVID-19 patients offer additional systemwide collaboration opportunities.
The COVID Recovery Center team also works closely with primary care providers for referrals, serving as a centralized resource to patients and providers who are struggling with the management of long-term symptoms, also known as post-acute sequelae. In addition, the center plans to launch peer support groups to allow patients to connect with each other and share their experiences in a safe space.
An estimated 10 to 20 percent of people who had COVID-19 experience persistent symptoms long after their infection has resolved, Levy said. In addition to the symptoms that patients like Vaughan encounter, COVID-19 can also cause the immune system to have a long-term inflammatory response that may lead to serious consequences for the heart, lungs, kidneys and other organs.
“We’ve always known that surviving a critical illness isn’t the same as recovering,” said Daniela Lamas, MD, co-director of the COVID Recovery Center. “Our hope is that this isn’t a chronic condition but rather a lingering condition that improves over time. We are trying to not only respond to it but also find ways to help people improve.”
As part of a broader commitment to health equity, the COVID Recovery Center hopes to partner with community organizations to remove barriers that may prevent patients from disadvantaged communities from seeking care.
“The shared vision we all had was to ensure we were serving the patients who were acutely affected by this pandemic,” said Ann-Marcia Tukpah, MD, MPH, a clinical fellow in Pulmonology who was involved in drafting the proposal for the center last year. “We want to make sure that every element of how care is provided in the center confronts these inequities. It’s not enough to just have the center — we have to think about improving awareness, engaging patients in a thoughtful way, considering transportation costs, the prospect of multiple visits and so on. We have to first identify these barriers, then develop processes to eliminate them.”
In addition to providing clinical services, the center will also include a robust research component to advance our understanding of the long-term impact of COVID-19 from pulmonary, vascular, immunologic, neuropsychiatric, psychological and social perspectives. Patients will be invited to enroll in clinical trials and a clinical research registry.
“There’s a lot we don’t know about this disease,” said Elizabeth Gay, MD, director of the COVID Recovery Center. “Being able to see patients in a setting where other clinicians and providers are thinking about a similar set of issues can allow us to identify patterns and understand needs. And from a research perspective, that offers the ability to develop a cohort you can follow to try to answer some of these questions.”
For patients like Vaughan — who began receiving care at the Brigham prior to the center’s establishment — the prospect of getting answers, and hopefully relief from her symptoms, might be that much closer.
“My body is not the same as it was before,” she said. “It feels like I don’t know myself anymore. It is unsettling to have the body you’ve been in for 31 years feel like a complete stranger. And I don’t know if I’ll go back to normal or this is just the new normal — but I hope not.”




 “It needed to be multidisciplinary because everybody’s expertise was needed,” Dias said.
“It needed to be multidisciplinary because everybody’s expertise was needed,” Dias said.















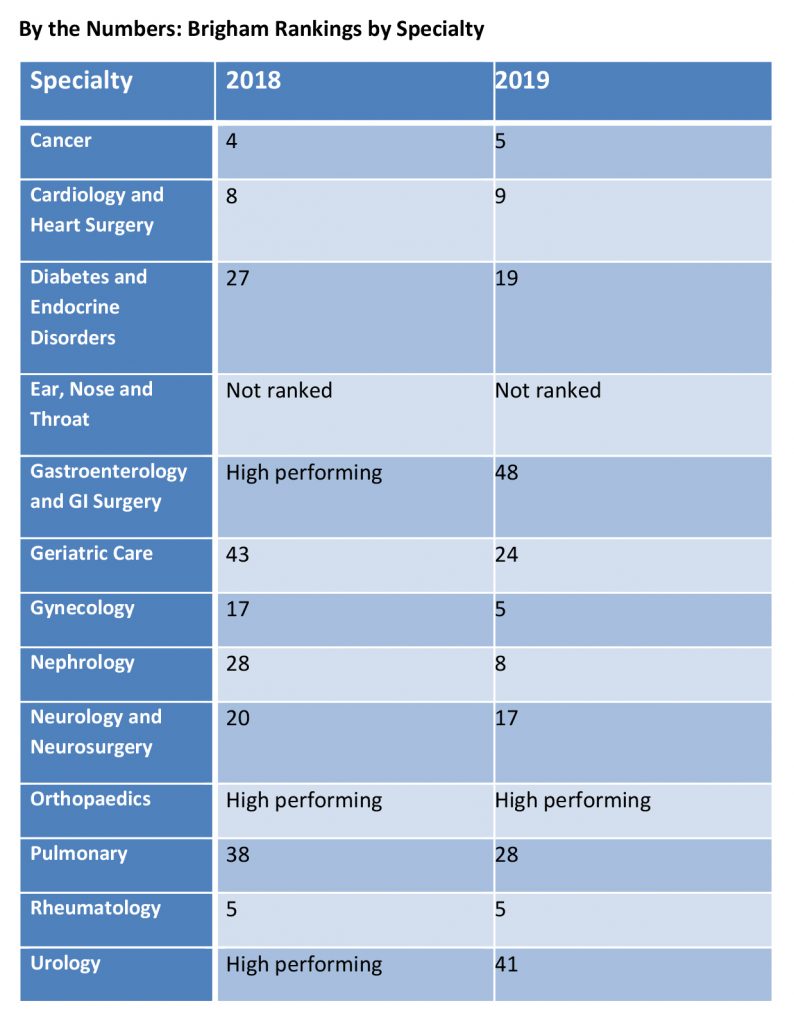
 Brigham and Women’s Hospital rose to No. 13 on the 2019 U.S. News & World Report’s ranking of Best Hospitals, up from No. 20 in last year’s annual Honor Roll. The Honor Roll is a distinction awarded to 20 hospitals that deliver exceptional treatment across multiple areas of care.
Brigham and Women’s Hospital rose to No. 13 on the 2019 U.S. News & World Report’s ranking of Best Hospitals, up from No. 20 in last year’s annual Honor Roll. The Honor Roll is a distinction awarded to 20 hospitals that deliver exceptional treatment across multiple areas of care.